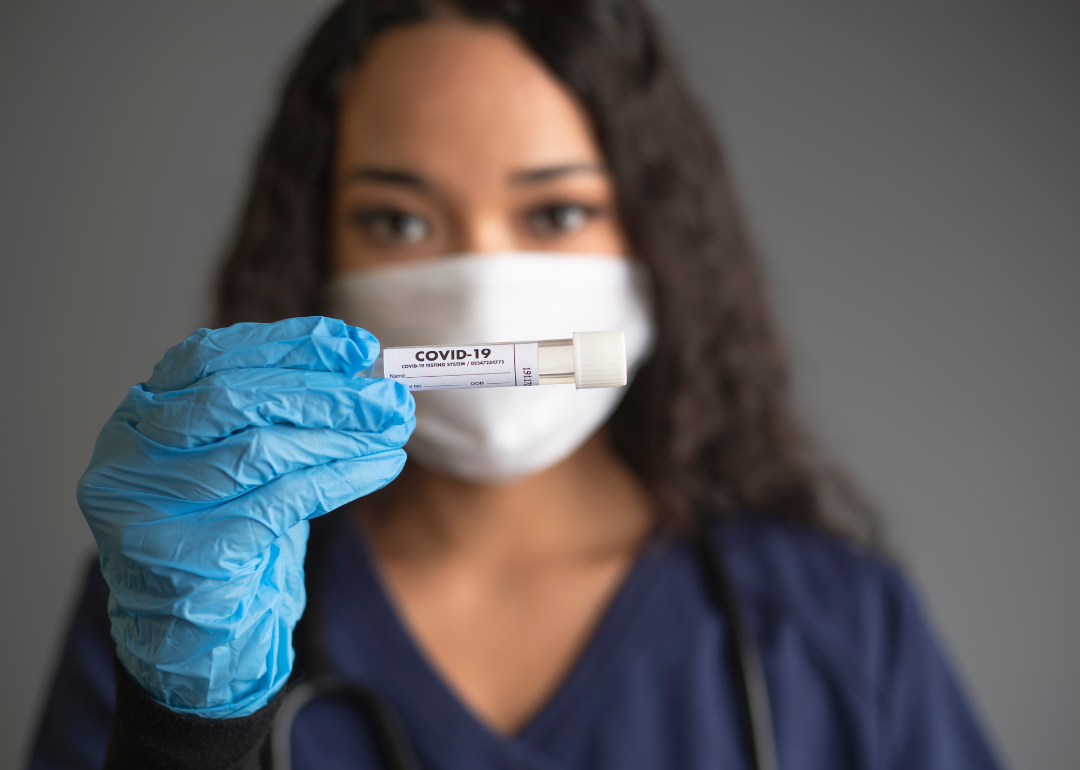
50 COVID-19 terms to know
When COVID-19 became a global pandemic, news junkies and casual observers alike were inundated with new terms and concepts. If you don't have a background in public health or epidemiology, however, these specialized terms can understandably be a bit hard to comprehend. Yet confusion is the last thing needed in a public health emergency. If a portion of the community doesn't fully grasp what needs to happen to stop the spread, consequences can be deadly. To help demystify some of the language related to the pandemic, Stacker used a variety of news reports and public health sources to compile a list of 50 terms that you need to know to understand COVID-19 news.
After the pandemic, you will never think the same way about face masks or hospital beds. Many members of the American public will also embrace a newfound understanding of virus transmission, hand-washing, and proper disinfecting methods from this experience. Whether you already had a rudimentary understanding of medical terms or wouldn't recognize an N95 face mask if you were handed one, brushing up on these 50 COVID-19 terms to know will undoubtedly help you understand the pandemic a bit better. Read on to find out what a PCR test is, what constitutes herd immunity, what it really means to flatten the curve, and more.
You may also like: States getting the least (and most) sleep
Virus
Perhaps the first concept to understand is a virus. These microscopic organisms can live outside of a host, meaning they can be transmitted on surfaces or by air. One particular virus—SARS-CoV-2—is responsible for the disease known as COVID-19.
[Pictured: This digitally colorized, negative-stained transmission electron microscopic (TEM) image depicts a number of Influenza A virions.]
SARS
Severe acute respiratory syndrome, or SARS, is an illness caused by a coronavirus called SARS-CoV—importantly, a different coronavirus than the one that causes COVID-19. This virus originated in horseshoe bats, and the infectious disease known as SARS first appeared in humans in 2003. Though there is no vaccine for SARS, no outbreaks have occurred since 2003.
[Pictured: This illustration, created by the CDC, reveals ultrastructural morphology exhibited by coronaviruses.]
MERS
Like SARS, Middle East respiratory syndrome, or MERS, is also caused by a coronavirus. The specific virus—MERS-CoV—typically passes from animals to humans, and human-to-human transmission is rare. Most infections occur after contact with dromedary camels and nearly 80% of the worldwide cases were recorded in Saudi Arabia.
[Pictured: Produced by the National Institute of Allergy and Infectious Diseases, this highly magnified, digitally colorized scanning electron microscopic image revealed ultrastructural details at the site of interaction of numerous (yellow) MERS-CoV viral particles located on the surface of a (blue) Vero E6 cell.]
SARS-CoV-2
The novel coronavirus that causes COVID-19 is known as SARS-CoV-2. While this virus is similar to the coronaviruses that cause SARS and MERS, it remains distinct. Research into exactly how the virus operates and infects humans is still ongoing.
[Pictured: Visualization of COVID-19.]
COVID-19
Short for Coronavirus Disease 2019, COVID-19 is how most people refer to the infectious disease caused by SARS-CoV-2. Common symptoms include fever, cough, shortness of breath, fatigue, headache, sore throat, and nausea.
Antibodies
Antibodies play a crucial role in the immune system. The body releases these proteins into the bloodstream when it detects a particular virus or microbe that it deems a threat. Since antibodies develop after a person is exposed to a virus, scientists believe they may offer some protection from the same virus in the future, though it’s unclear to what degree COVID-19 antibodies can protect against future illness.
[Pictured: Computer illustration of influenza viruses coated with antibodies (white); antibodies bind to specific antigens.]
Antigens
Antigens are proteins on a virus or germ that our immune system labels a threat, triggering an antibody response. Though testing for the presence of antigens can be a useful way to diagnose infectious diseases, scientists have not yet been able to find a unique protein target for COVID-19.
[Pictured: A chimeric antigen receptor molecule (light blue) binds to CD19 molecules (magenta) on a leukemia cell, activating a tyrosin kinase (red). The final result is the apoptosis of the cancer cell.]
PCR test
Polymerase chain reaction tests, or PCR tests, reveal whether or not a patient currently has a disease such as COVID-19. These tests search for the presence of the virus in the nose, throat, or respiratory tract.
Antibody test
Unlike PCR tests, serology tests, also known as antibody tests, check for the presence of antibodies in the bloodstream to determine whether or not a patient has had an infection in the past. Scientists think antibody tests may eventually determine whether or not a person will have immunity to COVID-19, but don’t yet know the level of antibodies needed to confer immunity.
Antigen test
Antigen tests offer similar info to molecular tests, and within as little as 15 minutes following a nasal or throat swab. Antigen tests, which detect small pieces of the novel coronavirus that trigger immune system response, are less sensitive than PCR tests: If a patient has COVID-19 symptoms but a negative antigen test result, it is recommended they get a PCR test to be certain they don’t have the virus. However, when it comes to a positive test result, antigen tests are highly accurate. This test is less expensive and complex, and faster than the other two types of approved diagnostic tests (molecular and PCR), so it can be useful in testing the masses; some experts predict that these tests may be widely available by this winter.
You may also like: What we know about children and COVID-19
False positive
A false positive is a conclusion that something is true when it actually isn’t. During the current pandemic, anecdotes of false negatives and false positives have popped up in the news, indicating that the PCR tests aren’t perhaps as reliable as scientists might hope.
False negative
Receiving a COVID-19 test with a false negative result means the test results indicate the patient does not have the virus when in fact they do. If a patient with COVID-19 symptoms has a negative antigen test result, but a positive PCR test, the antigen test may have delivered a false negative.
Epidemiology
This branch of medical science has received a lot of buzz during the COVID-19 pandemic. Epidemiology refers to the scientific study of the causes of health outcomes of the population at large, including environmental factors, infectious diseases, injuries, and natural disasters.
Disease modeling
Data scientists use mathematical models to calculate everything from cattle growth in a region to planetary motion, so why not use it to estimate the spread of COVID-19? Though several mathematical models for the pandemic—also known as disease models—exist, they vary wildly because scientists don’t have clear data on how many people have been infected, the infection rate, or the fatality rate.
WHO
One acronym that’s been seen all over the news is WHO, which stands for the World Health Organization. This international organization seeks to build a healthier global future and fight diseases throughout the world with the help of its 194 member states.
CDC
Another acronym dominating the news cycle in the United States is the CDC, or Centers for Disease Control and Prevention. This government agency has led the COVID-19 response in the United States by advising the highest levels of government, publishing consumer guides to social distancing and other hot topics, collecting data on the outbreak within the United States, and more.
[Pictured: The David J. Sencer CDC Museum located on the Edward R. Roybal campus in Atlanta, Georgia.]
HHS
The Department of Health and Human Services (HHS) is the overarching branch of the federal government focused on health functions as the parent organization for the CDC and National Institutes of Health (NIH). The HHS will be taking an “America First” approach to distributing the future vaccine, according to Sept. 2 statements by senior HHS official Garrett Grigsby to the press.
Pandemic
Although the words “pandemic” and “epidemic” sound quite similar, there’s an important distinction. While an epidemic is an outbreak that spreads quickly and infects many people at once, a pandemic is a type of epidemic that affects an even greater number of people over a larger geographic area. As COVID-19 has spread worldwide, it’s been classified as a pandemic.
[Pictured: The World movie theater using its name to send a deeper-meaning message about the COVID-19 pandemic with its sign, "The world is temporarily closed."]
Asymptomatic carrier
Much of the anxiety around COVID-19 centers on the fact that evidence suggests people can carry and transmit the disease while displaying few or no symptoms—in other words, they’re asymptomatic carriers. The realization that the virus can spread before you even realize you’re sick led to recommendations around social distancing, self-isolation, and even quarantine.
Community spread
Also known as community transmission, community spread refers to the circulation of a disease within the population of a certain area with no clear connection to an infected patient. For example, a health care worker who contracted COVID-19 after caring for patients with the disease would not qualify as community spread, but a city dweller who tested positive without knowing anyone who had COVID-19 would.
Droplet transmission
Sneezing, coughing, and even speaking produces respiratory droplets that can carry germs and viruses, including COVID-19. When diseases spread through these droplets, it’s known as droplet transmission. According to the WHO, droplet transmission is one of the primary methods of contracting COVID-19.
Fomite
Coffee cups, blankets, cardboard boxes, and countless other objects could all become fomites—or vehicles for the transmission of infectious diseases. Though fomites could potentially spread COVID-19, the CDC believes transmission from surfaces is less common than droplet spread.
Disinfectants
Demand for bleach, isopropyl alcohol, and other disinfectants skyrocketed early in the pandemic, as these household disinfectants can kill the SARS-CoV-2 virus on surfaces. That said, disinfectants are not safe to ingest, inhale, or spray on the body.
Flatten the curve
Picture a line graph: A tall, triangular shape indicates numbers rising quickly, then falling equally fast, while a gradual, flatter curve indicates a slower rise, plateau, and fall. When this graph represents COVID-19 cases, the skyrocketing cases in the first scenario would overwhelm the health care system, but the more gradual increase in the second scenario would conserve medical resources. Flattening the curve refers to controlling the spread of COVID-19 to create the second, more preferable outcome.
Herd immunity
This concept of herd immunity follows that if enough people get COVID-19, and the survivors build up antibodies that make them immune to future infections, the virus won’t be able to find new hosts and will die out slowly. Some countries are banking on this idea as a way out of the current pandemic.
[Pictured: Family walking at Macau's Senado Square wearing protective face masks due to the COVID-19 outbreak.]
Immunocompromised
People whose immune systems aren’t able to fight off infections as well as their peers’ immune systems would be considered immunocompromised. Cancer treatment, organ transplants, history of smoking, and diabetes are just a handful of the conditions that can cause someone to become immunocompromised.
Incubation period
After a virus enters the human body, it incubates for a period of time before symptoms appear. For COVID-19, the incubation period is usually between two and 14 days, and patients can still be contagious during that time.
Super-spreader
Although scientists don’t know exactly why, super-spreaders have the power to infect an unusually large amount of people with a disease. Thanks to super-spreaders, 20% of infected patients can drive up to 80% of new infections.
Viral shedding
Viral shedding is the period of time when a virus is being emitted by a host after replicating. According to a German study published in March, COVID-19 patients can shed high amounts of the virus before they even realize they’re sick.
Reproductive rate R0
The basic reproduction number—also known as R0, pronounced R-naught—represents the average number of people who will catch a disease from an infected person. If it’s greater than 1, the infection will likely continue to spread; when it falls below 1, the infection will likely start to fizzle out.
Test positivity rate
The test positivity rate indicates the percentage of people tested for a disease that actually test positive. For example, during the week of June 6, the national test positivity rate for COVID-19 was 6.3%, according to the CDC.
Comorbidity
A person with two or more illnesses at the same time has comorbidity. Obesity, hypertension, and diabetes are three comorbidities that can contribute to worse health outcomes in COVID-19 patients.
Intensive care unit
Patients who require advanced respiratory support, among other care, might be transferred to the intensive care unit (ICU). COVID-19 patients who need to be put on a ventilator often end up in ICUs, and many stay longer than the average three or four days.
Ventilator
U.S. hospitals faced a massive shortage of ventilators in the spring of 2020. These are medical devices that help people breathe if they’re unable to do so on their own. About 25% of all critically ill COVID-19 patients will need a ventilator.
Convalescent plasma therapy
This experimental medical treatment uses plasma from a recovered COVID-19 patient to treat someone who is currently sick with the disease. Though researchers don’t know how effective this therapy is yet, they hope it can help patients with severe symptoms fight the virus as well as help more moderate cases recover more quickly.
Personal protective equipment
Personal protective equipment, or PPE, refers to the face masks, N95 respirators, face shields, gloves, gowns, and other coverings that health care workers use to prevent the spread of COVID-19. A shortage of PPE hamstrung hospitals in the spring of 2020, and the U.S. Food & Drug Administration (FDA) anticipates that the supply chain will continue to be stressed for the remainder of the pandemic.
N95 respirator
Also known as an N95 mask, this form of PPE looks like a face mask that forms a tight seal around the nose and mouth. Not only does the material filter out 95% of the particles in the air, but the N95 respirator also requires a special 20-minute fit test to ensure it works properly.
Patient outcomes
Patient outcomes just refer to the end result of medical treatment on a patient, and this concept is used to evaluate the quality of medical care. A patient’s safety, satisfaction, and status help determine the patient outcome.
Clinical trial
Clinical trials are a crucial step in the development of any medication—including a potential COVID-19 vaccine. Vaccine trials typically occur in three phases: a small group trial to assess safety and immune system response, a much larger randomized trial, and efficacy or safety testing with thousands of patients.
Randomized trial
In a randomized trial, patients are randomly assigned into either an experiment group or a control group. The outcome being studied should be the only difference between the two groups.
Peer review
Peer review is a crucial component of academic publishing. Scientific journals rely on academics and experts reviewing one another’s articles to both weed out errors and improve the strength of an article under consideration. However, peer review takes time—anywhere from four weeks to six months—and some experts say the public can’t afford to wait that long for crucial information about COVID-19.
Preprint
Scholars and experts who aren’t willing to wait for their work to be peer reviewed often turn to preprint servers to make their manuscripts available right away. Also known as unrefereed preprints, these services publish work before it is peer reviewed or certified by a journal.
Contact tracer
Another important part of the fight against COVID-19 is contact tracing. This process traces and monitors all of the people who had contact with an infected person to ensure everyone who was exposed quarantines. Effective contact tracing could slow the spread of the virus.
[Pictured: The CDC activated its Emergency Operations Center to coordinate with WHO, federal, state and local public health partners, and clinicians in response to COVID-19.]
Essential worker
When governors across the United States issued stay-at-home orders for their constituents, one category of worker was often given an exception: essential workers. This category includes health care professionals, grocery store employees, public transportation workers, and other employees whose jobs were deemed crucial to the community.
[Pictured: A bus driver for the public transit system, an essential worker during the COVID-19 pandemic.]
Excess deaths
In epidemiology, the concept of excess deaths refers to the difference between the normal number of deaths and the reported number of deaths. Measuring the number of excess deaths is another way to estimate how many people have been killed by COVID-19.
[Pictured: A tally of deaths, confirmed cases, and other key metrics at one point during the COVID-19 pandemic.]
US Food & Drug Administration approval
The FDA must provide official approval for a new drug or biologic before it can be marketed in interstate commerce. Simply put, FDA approval means the agency has decided that the potential benefits of a drug outweigh the known risks.
Hydroxychloroquine
Commonly used to treat malaria, rheumatoid arthritis, and lupus, this drug came into the spotlight as a potential treatment for COVID-19 in March when the FDA granted an emergency authorization for its use during the pandemic. However, subsequent clinical trials found that hydroxychloroquine may not be effective after all, and the FDA revoked its authorization on June 15.
Remdesivir
Though biotech company Gilead Sciences first began researching remdesivir as a potential treatment for hepatitis C in 2009, the drug recently rose to prominence for its possible use against COVID-19. Remdesivir has broad-spectrum antiviral activity, so experts think it could potentially improve recovery time for COVID-19 patients. Preliminary studies on the drug’s efficacy, however, have had mixed results.
Racial disparity
A racial disparity refers to disproportionate differences among racial groups in regard to social constructs as seen in prison populations, health care, and employment rates in the U.S. (among others). During the pandemic, data show communities of color have been disproportionately affected by COVID-19. Black people are dying at a rate nearly twice as high as might be expected from their share of the U.S. population, according to the COVID Tracking Project. Additionally, the Navajo Nation has an infection rate per capita that’s higher than any U.S. state.
Surgeon general
Known as “the nation’s doctor,” the surgeon general takes responsibility for the health of Americans across the country, issuing advisories and reports about the latest scientific information. Currently, Vice Adm. Jerome Adams, M.D. serves as the 20th Surgeon General of the United States.
[Pictured: U.S. Surgeon General Jerome Adams speaks as President Donald Trump and Vice President Mike Pence look on during the daily briefing of the White House Coronavirus Task Force in the James Brady Briefing Room April 10, 2020, at the White House.]



